The current vocabulary for the use of patient data in care, treatment and research is complex and confusing. An important part of improving conversations about patient data is getting the words right, using words that are accurate but also accessible and meaningful. The words suggested here are the result of research commissioned by Understanding Patient Data, based on testing with the public and healthcare professionals.
Data or information?
‘Patient data’ and ‘Patient health information’ are the most effective overarching terms to use.
-
‘Patient data’ seems to be the easiest word for people to ‘get’.
-
There is no right or wrong: there are pros and cons for both and it may be helpful to adopt a dual approach using both ‘data’ and ‘information’, because different people respond in different ways to each phrase.
-
‘Data’ makes people think about numbers and codes, whereas information is broader.
- While there is a technical difference between ‘data’ and ‘information’, people use both words interchangeably.
-
Distinguish between information ‘for you’ and ‘about you’. Most people (both public and healthcare professionals) think ‘health information’ is information ‘for you’, for example a fact sheet or a patient information leaflet. The best way of avoiding this is to talk about ‘information from your patient record’.
-
Don’t use terms like ‘citizen’, ‘consumer’ and ‘user’ – our research suggested people much prefer the term ‘patient’.
-
Use data as a singular rather than plural. Even if plural is more accurate, most people now rarely say ‘data are…’.
-
Avoid using ‘personal’ in the overarching term, especially if the data may be used in an anonymised form. This can end up causing greater confusion if you end up with a term such as ‘anonymised personal information’.
Purposes for using data
‘Individual care’ works best to describe the use of data for a person’s own care and treatment.
-
The commonly used term ‘Direct care’ means nothing to anyone outside professional circles: people felt it sounded ‘ominous’, and conjured up images of an insurance company or credit cards.
-
The word ‘care’ works better than ‘treatment’ because it is broader.
‘Improving health, care and services through research and planning’ is the best phrase to use to describe the additional ‘purposes beyond direct care’ for which data may be used.
-
Although it is a long phrase, it helped give a sense of ‘the greater good’ and people wanted the specific detail to help understanding.
- This phrase ensures that there are ‘no surprises’ for people. All of the examples we trialled, including commercial access, academic research and NHS service improvements, were felt to fall under this umbrella term.
-
Phrases like ‘direct care’, ‘secondary uses’ and ‘purposes beyond direct care’ should only be used in technical conversations between professionals, rather than with the public and patients.
-
Don’t use ‘planning’ on its own. People thought it sounded like town planning or architecture or, in the context of the NHS, hospital closures.
Levels of identifiability
Many people express concerns that they might be identified when data is used. The technical language of identifiability is complex.
If you need to talk about whether someone could be identified from the data, take a look at our guide to large datasets, which includes an explanation of de-identification and terms like anonymisation and pseudonymisation.
Other hints and tips
-
Try to be clear about how much and what kind of data is used where possible. If you talk about ‘medical records’ people often envisage their entire medical record being passed on. Usually, only a subset of information contained within a record is used, such demographic information combined with diagnostic details.
-
Be careful with the phrase ‘data sharing’. It raises concerns that data is being openly released, rather than being used for a specific purpose with controls. A ‘data use contract’ may be more meaningful than a ‘data sharing agreement’.
- Using the word ‘your’. In focus groups, some thought it made the terms clearer, others thought it was too individualistic and pointed the finger at them. There are also concerns that using ‘your’ perpetuates the idea of ownership of data, and is particularly misleading if used in the context of ‘your anonymised information’.
This data glossary, produced by Connected Health Cities, also clarifies other technical terms around patient data.
Background research
These findings are based on research commissioned by Understanding Patient Data. Read our blog on the research and key findings. We asked Good Business to answer the question: what is the best vocabulary to use to talk about the use of data for care, treatment and research? They held a creative workshop with a range of language experts, and then tested the words and imagery with the public, patients and healthcare professionals, using quickfire focus groups.
Learn more from us
If you found this page helpful, you may be interested in this video about how to explain patient data to people. Grace talks through some tips and points to some more resources to help you.
Understanding Patient Data (UPD) has learnt a lot about how to communicate the way health data is used—whether that’s the right moments to choose or the right words to use.
So here are some of the things we think are most important to consider for designing communications about patient data, and links to the resources we have to help.
1. Data isn’t something people are always interested in
For those of us that work in this space, it’s important to remember that data is not the most fun and interesting topic for most people. This is especially crucial to recognise in health. When people go to the doctor, they’re usually in need of care and support—they’re not looking for a conversation about how data from their medical records can be used. One of our research participants said "we hear the word data and we think, how boring".
2. … But data can be controversial too
The way that patient data used tends to get the most attention when something goes wrong. We did some research into how news stories about health data are covered in the UK media and (perhaps unsurprisingly) it’s the stories about problems that get the most coverage. So, it’s important that risks that could lead to controversy are openly recognised and transparently managed. Rumour and misinformation thrive in a vacuum: so it’s better to be open about the things people are concerned about, like the involvement of commercial companies for example. This can be tricky, especially when things are changing fast, as they have during the Covid-19 pandemic. But being open about risk and uncertainty can help build credibility and integrity.
3. It’s important to find the right time and context
Given that health data isn’t something people think about much (and it gets a lot of bad press which can raise people’s concerns), finding the right moments to communicate how it’s used is important. When you first explain to people how data from their health records can be used, a question they’ll often ask is ‘Why are you telling me this now?’. That question is much easier to answer when the use of data is relevant to the person’s context. And we know from our research that people tend to be more interested in the way data is used when it helps them learn more about their own health, condition(s) or care. We also know that there’s only so much you can explain at one time, without overwhelming people. The more detail you give, the more questions you’re likely to get, so....

Prototype blood test letter
4. Give people the option to ask questions or learn more
People have different levels of awareness, concern and interest in how data from their health records is used. Some people will just want a high-level description, to know about their choices and some explanation about the safeguards. Others will want all the details and have lots of questions. It’s important to cater to those different needs, and to always give people somewhere to go to find out more, or have their questions answered from a reliable resource.
5. Explain how data is kept safe
One of the first things that most people want to know about patient data is how it’s protected. This is kind of unsurprising, given that health data feels sensitive and personal. The way health data is accessed and used in the UK is highly regulated, with a range of legal, institutional and technical safeguards in place—have a look at our explainer for more information. But the collection and use of data will always have risks. As I mentioned earlier, it's better to be open about them and not overpromise. People are all too aware of the risks and tend to be skeptical if they’re not addressed openly. So, it’s better to talk about the steps taken to keep data safe and protect confidentiality, than to promise that data is ‘secure’. That can never be completely guaranteed.
6. Use plain English and explain tricky words
It can be hard to explain the way patient data is used without slipping into using jargon. So UPD did some research to find the best words to use to explain patient data and tested them with members of the public and healthcare professionals. For example, the term ‘direct care’ is often used by people working in health and care, but it doesn’t mean much to most people. It’s much better to say ‘individual care’ instead. Testing or co-designing your communications is always a good idea, to help make sure they’re accessible to your audiences.
7. Images can help with explaining complex ideas
Pictures, diagrams and animations can help with explaining tricky concepts. For example, one of the first things people often want to know about patient data is whether they can be identified. But anonymisation is a complex concept that even experts have trouble defining. So, we developed this image to help explain the broad idea in an accessible way. Like all our content, it’s available under a CC-BY license for you to use in your own communications.
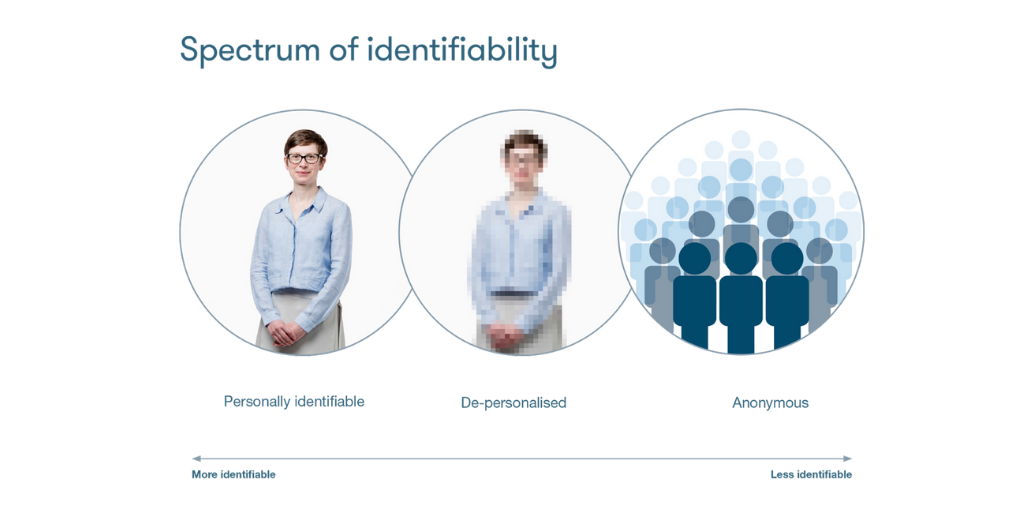
Use our content in your work
Take a look at the ‘Introducing patient data’ and ‘Research and resources’ sections on our site for more content you can use in your own work.
